2376-0249
Case Blog - International Journal of Clinical & Medical Images (2015) Volume 2, Issue 12
Author(s): Ali Raza Ghani*
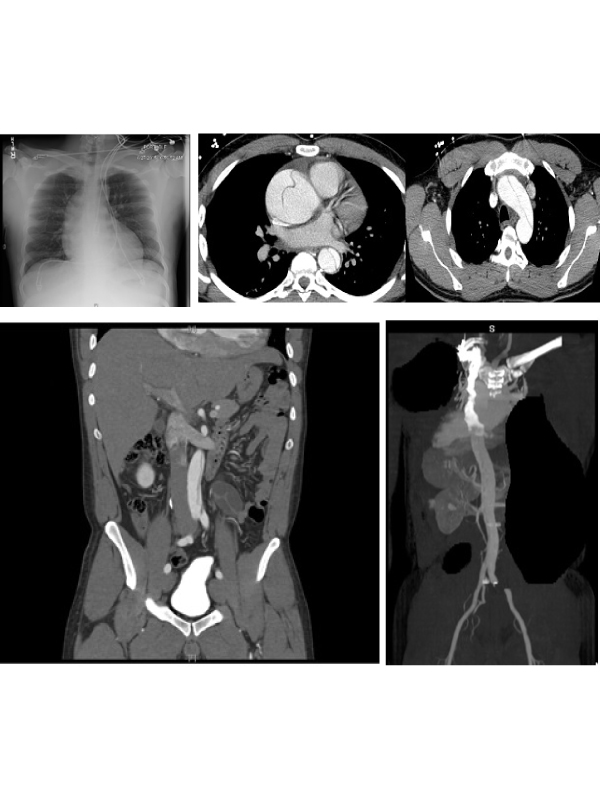
A 35 year old male with past medical history of hypertension presented with atypical chest pain. Emergency room vitals were HR 120/min, BP 173/73 mmHg and RR of 18/min on room air. Electrocardiogram showed atrial fibrillation with no ischemia. Physical exam showed irregular pulse, muffled heart sounds, and clear breath sounds. His heart rate converted back to normal sinus rhythm with Cardizem drip. Labs showed normal troponins and TSH. Chest X ray showed borderline widened mediastinum, CT angiogram chest demonstrated dilated aortic root (6.9 cm) with dissection extending from the aortic valve to the inferior thoracic aorta with cardiomegaly and pericardial effusion.
The CT angiogram abdomen showed dissection extending to proximal right common iliac artery (Figures 1-4). The patient was immediately taken to operating room with successful repair of dissection without any post-operative complication. Post-operative ECHO showed EF 55-60%.
 Awards Nomination
Awards Nomination

