2376-0249
Medical Image - International Journal of Clinical & Medical Images (2015) Volume 2, Issue 5
Author(s): Katherine Jeong and Daniel Jeong*
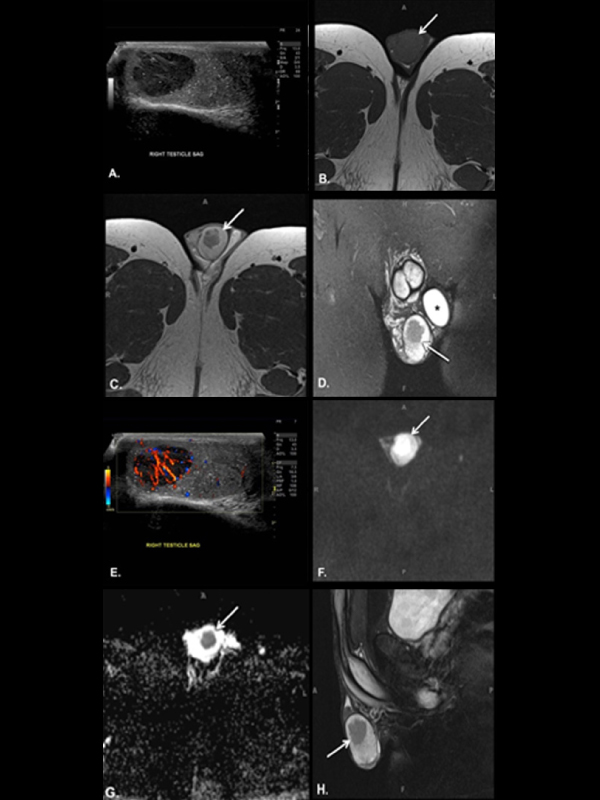
A 29 year old male with a history of left radical orchiectomy for nonseminomatous germ cell cancer with testicular prosthesis placement presented on follow-up with a new right testicular mass. Ultrasound and MRI revealed findings consistent with testicular seminoma (Figure 1). Right partial orchiectomy was performed, and surgical pathology of the tumor confirmed classic seminoma. No lymphovascular invasion was identified. The patient successfully completed adjuvant radiation treatment and remains stable on follow up. Testicular seminomas are germ cell tumors that are the most common nonhematologic malignancies affecting males 15-35 years old. Risk factors include undescended testis, previous tumor in the contralateral testis, and family history. Classic seminomas account for 85% of histological subtypes, while the remaining 15% are composed of anaplastic or spermatocytic subtypes.
They typically do not have specific serum markers and do not cause an elevated serum alpha fetoprotein. Ultrasound imaging characteristically reveals a well-defined homogeneous hypoechoic intratesticular mass with internal vascularity. On magnetic resonance, lesions show isointense T1 and hypointense T2 signal relative to testicular parenchyma with restricted diffusion. CT is important for staging and visualizing metastases, while FDG-PET may be used following treatment to monitor for metabolic activity within residual lymphadenopathy or extranodal metastases. Treatment involves orchiectomy for all stages. Stage I seminomas may be treated with active surveillance, adjuvant radiation therapy or single-agent carboplatin chemotherapy. Stage II or III seminomas are typically treated with radiotherapy, combination chemotherapy with bleomycin, etoposide and cisplatin, or both. Prognosis is good for all stages, with greater than 90% survival.
 Awards Nomination
Awards Nomination

