2376-0249
Clinical Image - International Journal of Clinical & Medical Images (2017) Volume 4, Issue 11
Author(s): Hosseininejad Seyyed-Mohsen1*, Gharib Mohammad-Hadi2, Hosseini Seyyed Ahmad*3 and Hosseininejad Fateme-Sadat4
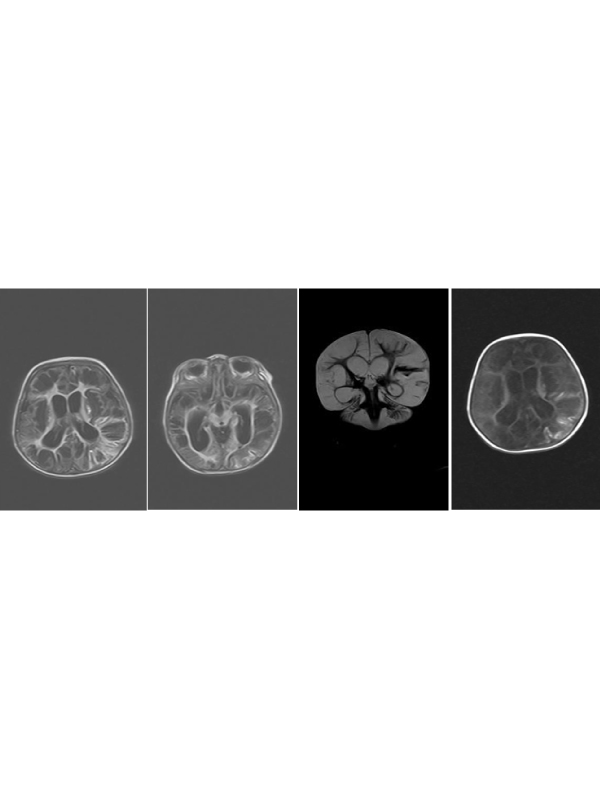
Clinical Image: A 7- month old male infant and a known case of cerebral palsy (CP) because of perinatal infection was referred to our academic Taleghani children hospital(Gorgan, Northern Iran), due to inability to intake food percutaneous insertion of gastrostomy tube was planned for him. In a retrograde investigation, we noticed his post natal brain Magnetic Resonance Imaging (MRI) (Figure 1). It illustrates severe hypoxic ischemic change of hemispheres, hydrocephalus, white matter signal abnormality predominantly in posterior regions esp. in parieto-temporal lobes and encephalomalacic cysts esp. in temporal poles;
His MRI also depicted atrophy of caudate nuclei and T2 hypersignal intensity of thalami. In addition to above radiologic findings, urine quantitative real-time PCR was positive for CMV with a DNA viral load of 143700 IU/ml. All these findings were highly suggestive for cystic encephalopathy due to CMV (TORCH classification) infection of the brain for this infant.
He was born symptom-free from repeated cesarean-section (RCS) of a term non-complicated pregnancy with a birth weight of 3900 g, appropriate for gestational age in a Turkmen family from a consanguineous marriage. His drug history consisted of phenytoin (5 mg/kg/day). CMV is the most common cause of intra-uterine infection and most common cause of congenital infective brain damage, occurring in 0.2-2.4% of live births. The vast majority (90%) of infected babies are asymptomatic at birth, but some may develop symptoms after 6-9 months [1].
Some of MRI findings include [2]:
• White matter lesions: Predominantly parietal or posterior white matter involvement
• Ventriculomegaly and subarachnoid space enlargement
• Delayed myelination
• Periventricular and temporal pole cysts
The Differential diagnosis include HIV encephalitis, progressive multifocal leukoencephalitis (PML) and primary CNS lymphoma (periventricular but has mass effect and enhances). Primary stabilizing measures were undertaken for our patient. No more abnormality was found in laboratory tests. His PEG tube was inserted successfully and the infant was discharged after acceptable clinical condition.
 Awards Nomination
Awards Nomination

