2376-0249
Clinical-Medical Image - International Journal of Clinical & Medical Images (2021) Volume 8, Issue 4
Author(s): Drissi Abdel-Ilah M, Retal Hamza, Hounayda Jerguigue, Rachida Latib, and Youssef Omor
Clinical Image
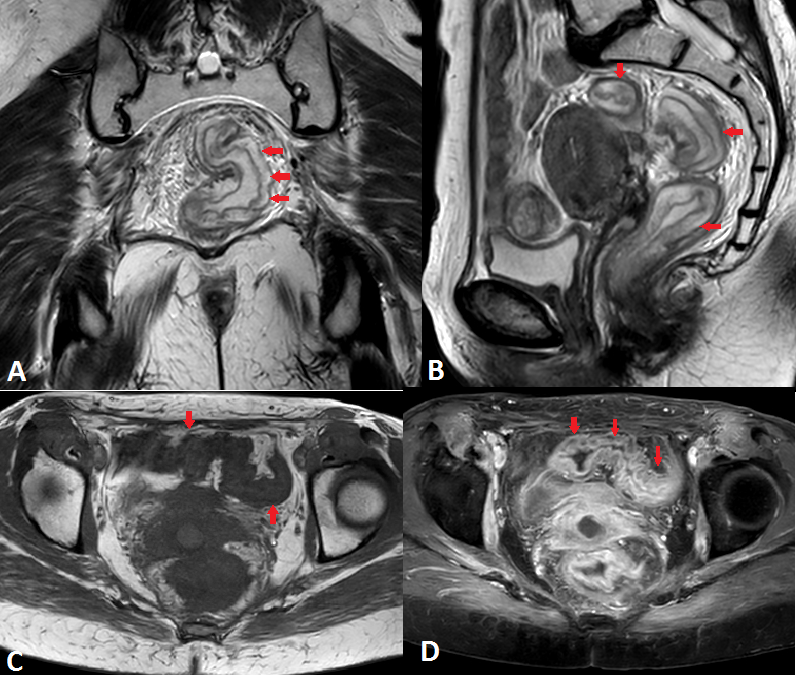
Radiation enteritis ou radiation enterocolitis (RE) is defined by the set of digestive manifestations involving the small intestine, colon and rectum occurring after abdominopelvic irradiation, markedly reduced since the development of new modern irradiation techniques but it can be favored by certain risk factors such as obesity, diabetes, Inflammatory bowel disease (IBD) as well as excessive irradiation. 5% to 15% of patients treated with radiotherapy (usually>4500 Gy) develop chronic enteropathy. The acute RE manifests mainly by an acute diarrhea around the 2nd week after irradiation and regresses 2 to 4 weeks after the end of radiotherapy, requiring a temporary interruption of treatment. The Chronic ER occurs 2 months to 30 years after the end of radiotherapy responsible for chronic constipation by digestive stenosis or diarrhea and under nutrition by malabsorption as well as abscesses, fistulization and ulcerations with rectal bleeding. CT and MRI mainly show thickening of the intestinal wall with diffuse sub mucosal mural edema responsible for narrowing of the lumen, sometimes complications such as obstructions and fistulas (Figures 1 and 2). The differential diagnosis arises mainly with tumor recurrence, IBD, digestive lymphoma or mesenteric ischemia. Medical treatment of Radiation Proctitis is based on Corticosteroid enemas, Endoscopic treatments (thermo coagulation, electrocoagulation) surgical treatment as a last resort in case of failure of medical treatment. Prevention is based on limiting the irradiation field, with identification of organs at risk and optimization of radiotherapy doses.
Keywords: Radiation enteritis; Radiotherapy; MRI
 Awards Nomination
Awards Nomination

