2376-0249
Case Blog - International Journal of Clinical & Medical Images (2015) Volume 2, Issue 6
Author(s): Ajay M*, Shaswati S, Jayanta S and Basu SK
Introduction Foreign bodies implanted in the Para pharyngeal space are quiet rare. Most cases occur in infants and children, and are usually accompanied by a poor and confusing history. Due to its rarity, it is not usually considered among the differential diagnosis of palatal lesions. This is a totally confusing history about a 6 months old child who presented with vague symptoms and was later diagnosed to have impacted metallic foreign body in the parapharyngeal space.
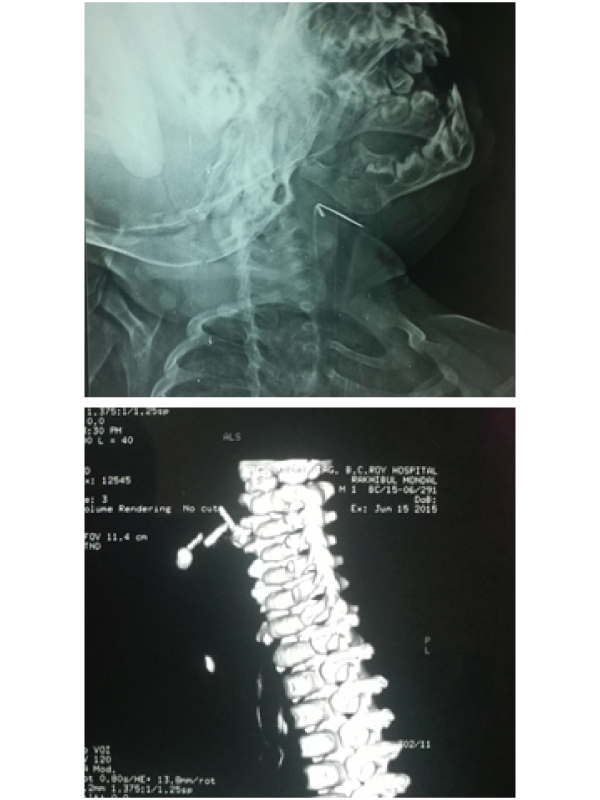
Case Blog A ten months old male child came to our ENT department with complaints of dysphagia in a child and complaints of irritability, decreased sleep. On examination child was little irritable. Paediatrics opinion was taken, general examination as well as systemic examinations revealed NAD. Suspecting foreign body of nasal cavity, X ray nasopharynx lateral view was advised. Surprisingly metallic foreign body was seen in the pharynx (Figure 1). On oral cavity examination, no haematoma or swelling was observed. Oral cavity was absolutely fine. To define the exact location of the foreign body, CT scan was adviced. CT scan revealed metallic foreign body in the left side parapharyngeal space (Figure 2). The patient was immediately admitted and was planned for foreign body removal under general anaesthesia. Tran’s oral approach was done and the metallic foreign body was removed. Wound repaired with vicryl 3-0 interrupting sutures.
Discussion The possibility of children inserting objects into their oral cavity is the main reason why palatal foreign bodies and injuries are most common in this age group [1]. The natural position of the tongue, thumb sucking and feeding patterns further led to the adherence of a foreign body to the roof of the oral cavity by producing a constant force on the foreign body up against the palate and also sometime it may enter the parapharyngeal space. Management of trauma to the palate and lateral pharyngeal wall will initially include hospitalisation, mucosal repair and antibiotic prophylaxis and also diagnostic studies as well as treatment if thrombosis or neurologic changes develop. Shanon et al. [2] recommended hospitalisation for 48 to 72 h, due to the devastating
 Awards Nomination
Awards Nomination

