2376-0249
Case Blog - International Journal of Clinical & Medical Images (2014) Volume 1, Issue 11
Author(s): Alexander KCLeung* and Benjamin Barankin
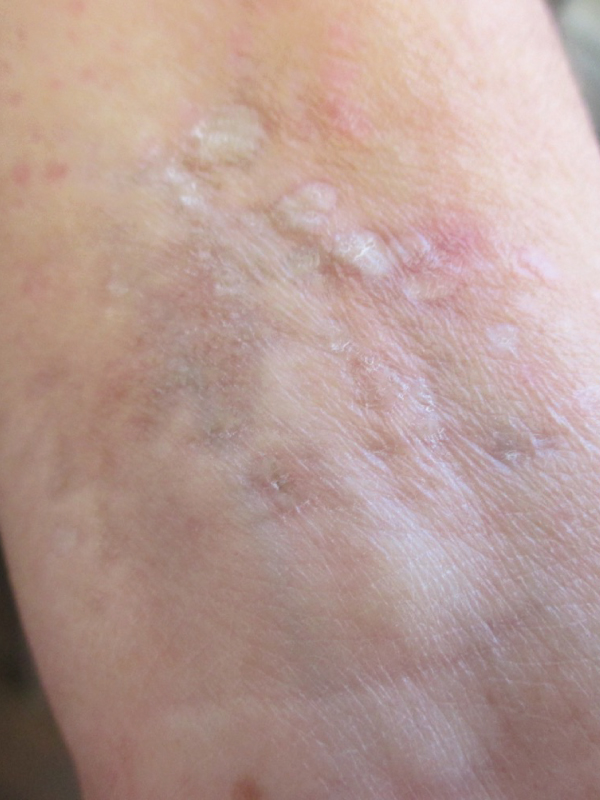
A 50-year-old woman presented with ivory-colored sclerotic lesions on the left wrist of 10 to 12 months’ durations. The lesions were asymptomatic but had gradually spread. She had alopecia areata and diabetes mellitus type 1. Her past health was otherwise unremarkable. No genital or oral lesions were noted. Lichen sclerosus (also called lichen sclerosus et atrophicus) is an autoimmune, chronic, progressive, inflammatory dermatosis that presents with sclerosis, atrophy, and pruritus predominately affecting the anogenital area. Approximately 6 to 15% of patients present with extragenital lesions. Similar to genital lichen sclerosis, extragenital lichen sclerosis is more common in females than males. The condition is rare in children. Classical sites of extragenital lesions are the neck, shoulders, back, abdomen, thighs, and wrists. Early lesions present as flat-topped, white or mildly erythematous, polygonal papules that progress into sclerotic, atrophic, ivory-white plaques or patches. In advanced stages, follicular plugging, peripheral erythema, and telangiectasia may be seen. The affected area often has a parchment-like or cellophane paper-like wrinkled surface (often termed cigarette paper wrinkling) that correlates with epidermal atrophy. Extragenital lichen sclerosus is usually asymptomatic but can occasionally be pruritic. Koebnerization is common at extragenital sites. The diagnosis is mainly clinical and can be aided by dermoscopy. Dermoscopy typically shows comedo-like openings that correspond to the histological findings of follicular plugging and whitish areas that correspond to the atrophy of the epidermis. A punch biopsy should be considered if the diagnosis is in doubt. The disease tends to run a chronic, progressive, protracted course with exacerbations and remissions. Spontaneous remissions are rare. Rarely squamous cell cancer has been reported within these lesions. Ultrapotent topical corticosteroids are the mainstay of therapy. Topical immunomodulators such as tacrolimus and pimecrolimus are not as fast-acting or effective as ultrapotent topical corticosteroids in the treatment of this skin condition, although they can be considered in the maintenance phase of treatment. Emollients should also be used to help repair the skin barrier.
 Awards Nomination
Awards Nomination

