2376-0249
Clinical-Medical Image - International Journal of Clinical & Medical Images (2016) Volume 3, Issue 12
Author(s): Melnichenko YM, Savrasova NA and Kabak SL
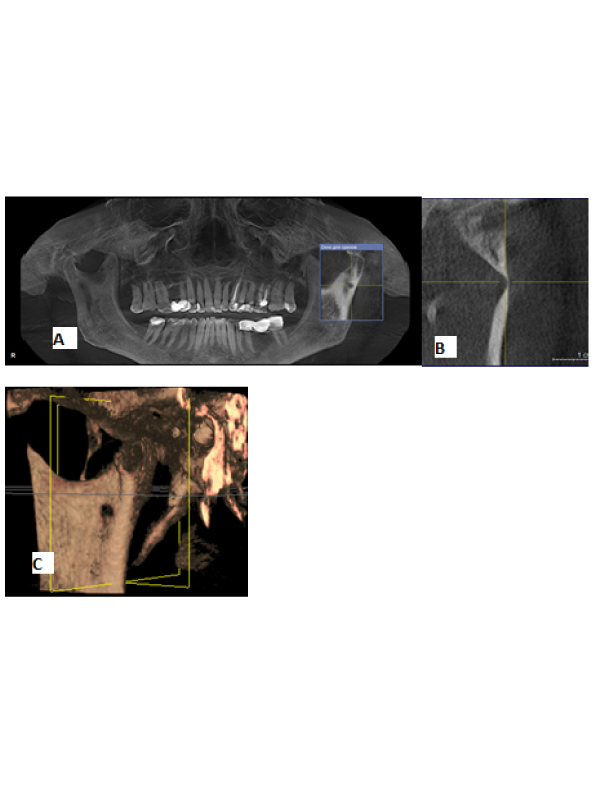
Case Presentation A 57-year-old Caucasian woman 11/28/16 was referred for cone-beam computed tomography (CBCT) examination for the prosthetic treatment planning. There were no complaints of pain or any other symptoms. She had no history of trauma, facial bones or temporomandibular joint diseases. CBCT scans were performed on Galileos GAX5 (Sirona Dental Systems, Bensheim, Germany) using standard settings (85 kV; tube current: 507 mA; acquisition period: 14 sec; effective radiation time: 2-6 sec; voxel size: 0.3 × 0.3 × 0.3 mm). Reformatted panoramic and sagittal CBCT images were analyzed using GALILEOS Viewer (Sirona, Bensheim (Germany). On reformatted panoramic images single round radiolucent area of size 9.10 × 7.93 mm of the ramus of mandible upwards and backwards from mandibular foramen was detected. 3D reconstruction showed ð local ramus thinning with the formation of the depression on its inner surface. Outer cortical plates were saved throughout. Radiological signs of bone lesion were not found. Contralateral ramus of the mandible was without pathological findings. In comparison with the appearance of the lesion 5 and 3 years ago, the shape and size of the lesion now did not show any distinguishable changes. Absence of the progression and unaltered structure of the jaw allowed excluding mass lesions.
Diagnosis Parotid Stafne bone defect (SBD) of the left mandibular ramus, lingual variant. According to the literature the overall incidence of SBD varies from 0.009% to 0.3% [1]. Wolf and Barker believe that SBD develops in the result of the pressure by hyperplastic/hypertrophic salivary glands tissues on the bone surface (Figure 1) [2,3].
 Awards Nomination
Awards Nomination

