2376-0249
Case Blog - International Journal of Clinical & Medical Images (2014) Volume 1, Issue 2
Author(s): Bahadir Sarli, Kayseri Education
Left Ventricular (LV) pseudoaneurysm is a rare complication of myocardial infarction which developes in leads to increased morbidity and mortality [1,2,3]. LV rupture limited by pericardium and in situ thrombosis is the chief point of pseudoaneurysm formation. Hence, LV pseudoaneurysm has a high risk for spontaneous rupture. Hereby, we present a matchless image of a giant left ventricular pseudoaneurysm mimicking the heart symbol which was described by Cro-magnons 28.000 years ago [4].
Case blog
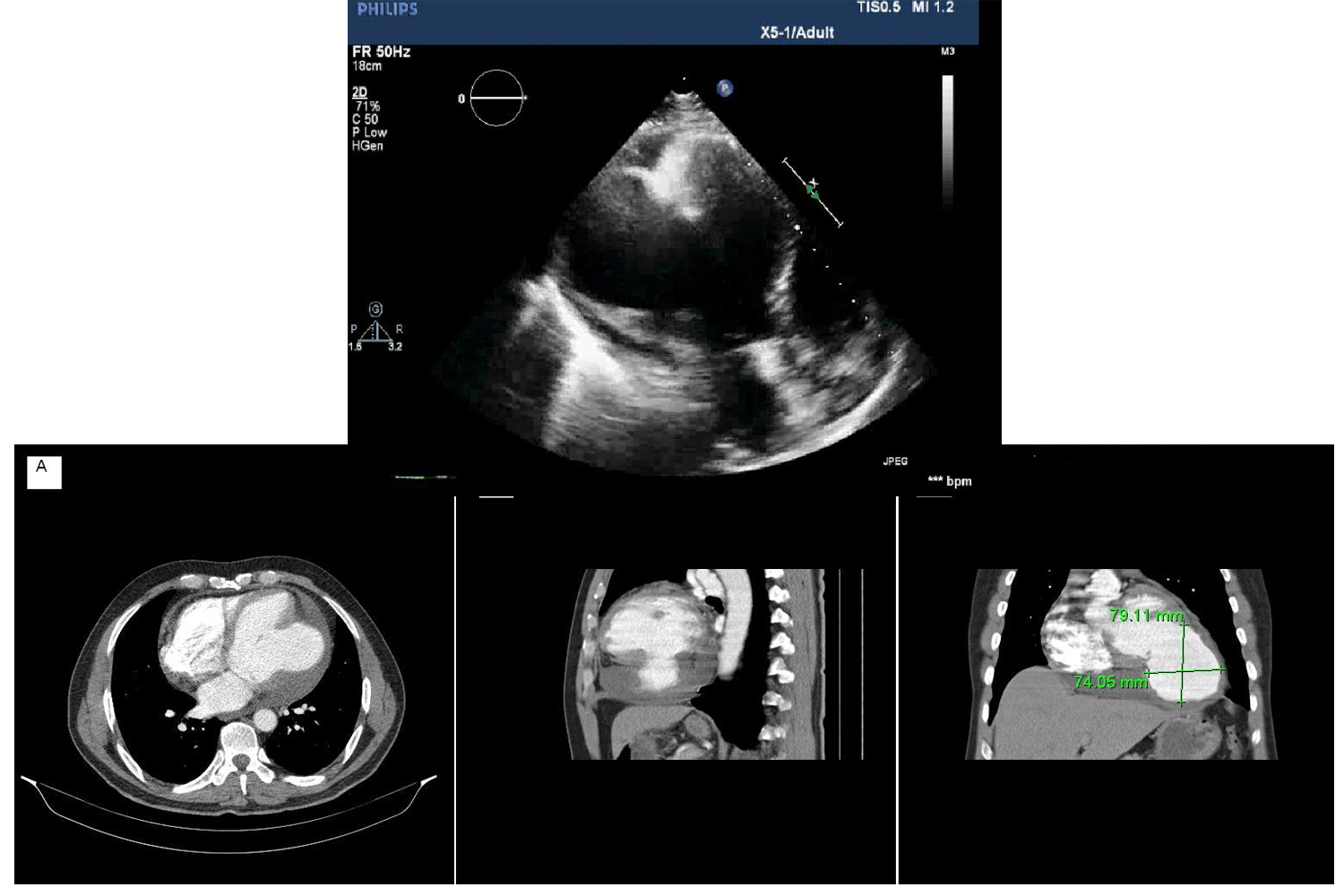
A 56 years old male patient was admitted to our clinic for acute heart failure. He had history of chest pain 1 week ago. There were bibasillary pulmonary rales and S3 in his physical examination. ECG revealed non-spesific ST and T wave changes. Troponin I level 0.33 ng/ml. Transthoracic echocardiogram revealed a huge 7x7 cm aneurysm of posterolateral wall with spontaneous echo contrast within the aneurysm (Figure 1). Multislice BT confirmed the presence of aneurysm (Figure 2). Coronary angiography revealed non-critical stenosis at left circumflex artery and left anterior descending artery (Figure 3). Our heart team considered that this aneurysm was probably due to a coronary event occured 1 week ago during patients chest pain. Medical treament targeting heart failure failed to relieve patients’ symptoms. Thus, patients was scheduled to repair surgery and transferred to cardiovascular surgery department. Postoperative period until discharge was uneventful.
Discussion
Left ventricular pseudoaneurysms usually develop as a consequence of transmural myocardial infarction. It is a potentially fatal complication of myocardial infarction which may progress to left ventricular free wall rupture in 30% to 45% of untreated patients [5]. In deed, LV pseudoaneurysm is a kind of LV free wall rupture limited by the overlying pericardium [6]. Having a neck that is narrower than the diameter of the aneurysm is the hallmark of LV pseudoaneurysm. Delayed revascularisation is the leading cause of pseudoaneurysm formation [7]. Transthoracic echocardiography is the most feasible way of diagnosing LV pseudoaneurysm. Although surgical mortality is high, it is still the most appropriate way of curative treatment in patients with LV pseudoaneurysm [8]. In this report, we presented a giant LV pseudoaneurysm mimicking the sign of love in a patient presenting with heart failure.
4. Puech PF1, Puech B (2012) Can we still hear the Cro-magnon man? Acta Med Hist Adriat 10: 331-338.
6. Kansiz E, Hatemi AC, Tongut A, Cohcen S, Yildiz A, et al. (2012) Surgical treatment of a giant postero-inferior left ventricular pseudoaneurysm causing severe mitral insufficiency and congestive heart failure. Ann Thorac Cardiovasc Surg 18:151-155.
8. Frances C1, Romero A, Grady D (1998) Left ventricular pseudoaneurysm. J Am Coll Cardiol 32: 557-561.
Corresponding author
Bahadir Sarli
Kayseri Education and Research Hospital
Department of Cardiology
Turkey
 Awards Nomination
Awards Nomination

